When your child is sick, it is without a doubt that you want to do everything that you can to help them feel better. However, it is important to understand that antibiotics are not always the answer. Antibiotics are strong medicines that may come with side effects and other risks that you might not be aware of. When a patient needs antibiotics, the potential benefits that the antibiotics will deliver outweigh these risks.
When is it appropriate for my child to receive antibiotics?
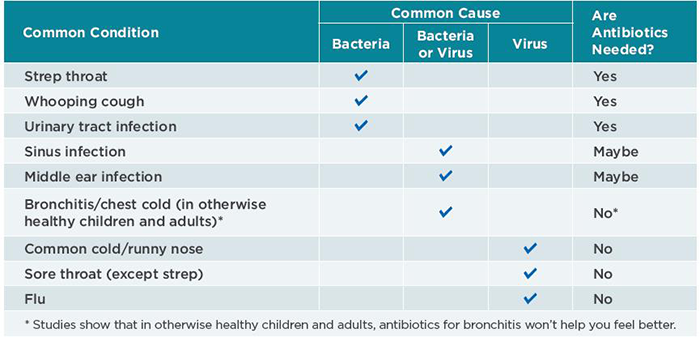
Most infections are caused by two kinds of germs: bacteria or viruses. Antibiotics can cure bacterial infections only. Some examples of bacterial infections are strep throat and some types of pneumonias. Some examples of viruses are the common cold, most coughs and the flu. Yellow or green mucus does not necessarily mean that your child has a bacterial infection; it is normal for mucus to get thick and change color during a viral cold. Using antibiotics for a virus will not cure the infection, help your child feel better or keep others from catching your child’s illness. Viral illnesses are typically self-limiting, meaning that your child can fight the infection without targeted medicine against the virus.
What’s the harm in giving antibiotics anyway, even if my child might not have a bacterial infection?
Antibiotics can cause some bacteria in your child’s body to become resistant, or unable to be killed with certain antibiotics. This can become a problem later for future potential infections and can also be spread to others. Generally speaking, many common infections are becoming resistant to antibiotics. An estimated 2 million illnesses and 23,000 deaths occur each year in the U.S. due to antibiotic-resistant infections. Overuse and misuse of antibiotics are main drivers of resistance, with an estimated greater than half of antibiotics being unnecessarily prescribed to children in doctor office settings for cough and cold illness.
Antibiotics can also cause side effects, such as diarrhea, nausea, skin sensitivity and even Clostridium difficile-associated diarrhea. These side effects and allergic reactions cause 1 out of 5 emergency department visits for adverse drug events and lead to 50,000 emergency department visits in children each year.
What should I do when my child is sick?
The Centers for Disease Control and Prevention (CDC) suggest three important questions to ask your healthcare provider when your child is sick:
- What is the best treatment for my child’s illness?
- What do I need to know about the antibiotics that you’re prescribing for my child today?
- What can I do to help my child feel better?
When your provider prescribes an antibiotic to treat a bacterial infection, be sure to ensure its use as directed. If your provider thinks that your child has a virus, symptom management with pain relievers, fever reducers, saline nasal spray or drops, warm compresses and increasing liquid intake should help your child on the road to recovery.
 https://riseandshine.childrensnational.org/wp-content/uploads/2026/05/hantavirus-feature.jpg
300
400
Rise and Shine
https://riseandshine.childrensnational.org/wp-content/uploads/2017/11/childrens_riseandshine_logo.jpg
Rise and Shine2026-05-13 10:07:552026-05-13 15:42:49What you need to know about hantavirus
https://riseandshine.childrensnational.org/wp-content/uploads/2026/05/hantavirus-feature.jpg
300
400
Rise and Shine
https://riseandshine.childrensnational.org/wp-content/uploads/2017/11/childrens_riseandshine_logo.jpg
Rise and Shine2026-05-13 10:07:552026-05-13 15:42:49What you need to know about hantavirus



















Leave a Comment
Want to join the discussion?Feel free to contribute!