What is hand, foot and mouth disease?
Hand, foot and mouth disease (HFMD) is a common childhood illness caused by a virus, known as coxsackievirus, which spreads easily from person to person. It can affect anybody, but it is most commonly seen in young children. HFMD tends to spread more during the summer and fall and can spread easily among young children in day care and preschools.
How do I know if my child has hand, foot and mouth disease?
Symptoms can include:
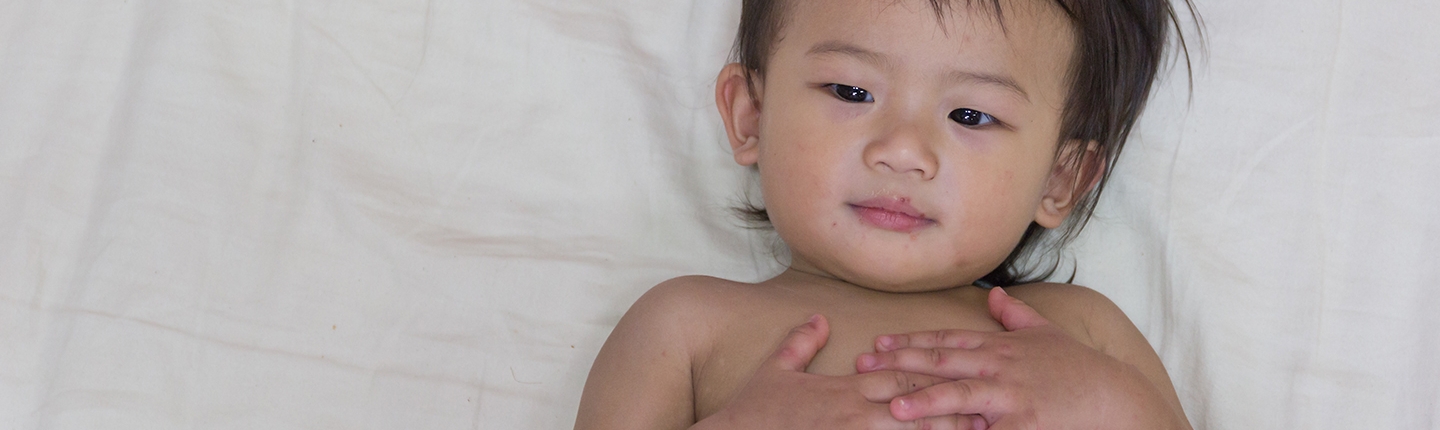
- Rash on the body consisting of small blisters that are nearly flat and often have a bright red rim. As the name implies, these spots appear most commonly on hands, feet, and around the mouth (more so than inside the mouth). The spots can occur on either side of the hands and feet. The strain of HFMD that we’re seeing in our area also involves the bony side of the elbows and knees, as well as the buttocks.
- For children with childhood eczema (atopic dermatitis), HFMD may spread to areas where there is underlying eczema.
- Low-grade fevers (typically less than 102 degrees)
- Sometimes there can be small, red sores in the mouth. They can be hard to see but they are painful, and that leads to decreased eating and drinking, as well as increased drooling.
Is hand, foot and mouth disease dangerous?
Most children with HFMD get better without any complications. The main risk is dehydration because children with painful mouth sores may refuse to eat or drink. This can usually be managed at home with over-the-counter pain medication. Serious complications are rare.
This year’s strain of HFMD has fewer instances of mouth and throat sores compared to older strains. About 2-3 months after a child has HFMD, he or she may experience painless shedding of several fingernails or toenails. Although dramatic, the nail shedding is both harmless and painless. New nails will be seen underneath the shedding nail and the new nail will grow in normally.
How is hand, foot and mouth disease treated?
HFMD goes away on its own, and because it is a viral illness, antibiotics will not work. You can, however, treat the symptoms.
The rash is usually not bothersome and does not typically need topical treatments. If the child has severe eczema and it seems like the rash is spreading to the raw, itchy areas, and if the child then develops a fever or is uncomfortable, please see your doctor. There are conditions, other than HFMD, that can spread quickly all over a child’s eczema and some of those require medical attention. You may treat and control your child’s pain and fever with the over-the-counter medications acetaminophen (such as Tylenol®) or ibuprofen (Motrin®/Advil®). Ibuprofen can be given to children over 6-months-old every six hours, and acetaminophen can be given every four hours. Some children experience the most relief from alternating these medications every three hours (for example, give acetaminophen, then three hours later ibuprofen, then acetaminophen three hours after that, and so on).
Do not wake your sleeping child to provide medications, but if they wake up uncomfortable, treat them. It is okay if your child does not want to eat much while they are sick, but they do need plenty of fluids. Cold fluids often feel good on sore throats. Avoid citrus and salty foods.
As the small blisters start to dry up, the skin looks like it has shiny dried spots of red-brown paint. Those spots will clear up on their own and will not leave any scars or discoloration behind.
When should I call my child’s primary care provider?
If you are worried, you are never wrong to call or make an appointment with your child’s provider. Call your pediatrician immediately if your child:
- Is dehydrated: Look for dry lips and mouth or decrease in urine output (your child should make urine at least every six hours)
- Is listless or you are concerned about how sick your child looks, especially if he/she does not perk up after a dose of ibuprofen or acetaminophen
- Has a stiff neck
- Has a fever above 105 degrees, a fever that lasts more than two to three days, or is younger than 3 months old with a fever higher than 100.3 degrees
Remember: if your child’s fingernails or toenails seem to be coming off a couple months after having HFMD, don’t worry. You don’t need to see your doctor for this unless the child is in pain or the skin around the nails looks infected.
How long is my child contagious?
Children are most contagious at the beginning of the illness. Although viruses may last longer, children can go back to child care once the fever has been gone for 24 hours and they don’t have open sores. I typically recommend waiting to return to child care until after the rash stops spreading, but it does not have to be completely gone. The rash will slowly fade over the course of a week or so. Hand washing, disinfecting surfaces and shared objects, and limiting close contact with infected individuals are the best ways to help prevent transmission.
 https://riseandshine.childrensnational.org/wp-content/uploads/2026/05/hantavirus-feature.jpg
300
400
Rise and Shine
https://riseandshine.childrensnational.org/wp-content/uploads/2017/11/childrens_riseandshine_logo.jpg
Rise and Shine2026-05-13 10:07:552026-05-13 15:42:49What you need to know about hantavirus
https://riseandshine.childrensnational.org/wp-content/uploads/2026/05/hantavirus-feature.jpg
300
400
Rise and Shine
https://riseandshine.childrensnational.org/wp-content/uploads/2017/11/childrens_riseandshine_logo.jpg
Rise and Shine2026-05-13 10:07:552026-05-13 15:42:49What you need to know about hantavirus











Leave a Comment
Want to join the discussion?Feel free to contribute!