Sickle cell disease is an inherited blood disorder that affects approximately 100,000 Americans, according to the Centers for Disease Control and Prevention (CDC). The disorder is characterized by defective hemoglobin, a protein in red blood cells that carries oxygen to the tissues of the body.
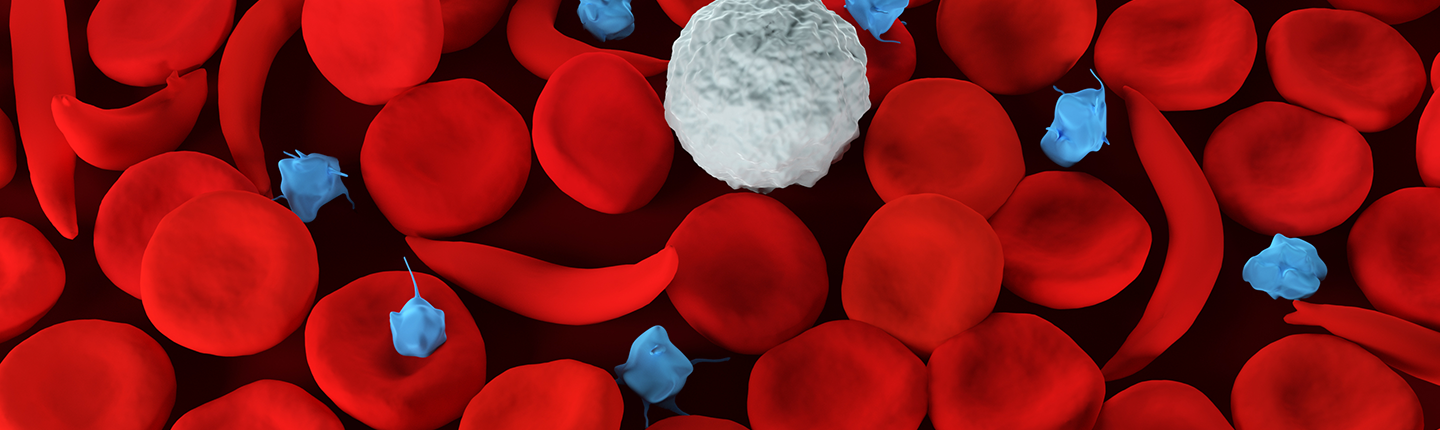
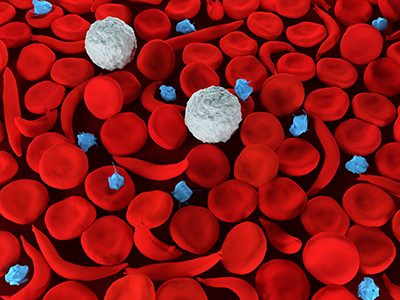
Normal red blood cells are smooth, round and flexible, like the letter “O,” so they can move through the vessels in our bodies easily. Sickle cell red blood cells are stiff and sticky, and form into the shape of a sickle, or the letter “C,” when they lose their oxygen. These sickle cells tend to cluster together, and cannot easily move through the blood vessels. The cluster causes a blockage in small arteries or capillaries and stops the movement of healthy, normal oxygen-carrying blood. This blockage is what causes the painful and damaging complications of sickle cell disease.
Although sickle cell disease primarily affects people of African descent and Hispanics of Caribbean ancestry, the trait has also been found in those with Middle Eastern, Indian, Latin American, American Indian and Mediterranean heritage.
Sickle cell disease symptoms
Sickle cell disease can be diagnosed with a simple blood test during routine newborn screening tests in hospitals.
Symptoms and complications of sickle cell disease may include, but are not limited to:
- Excruciating bone pain
- Anemia
- Jaundice
- Acute chest syndrome
- Stroke
Treating sickle cell disease
Specific treatment for sickle cell disease and its complications will be determined by your child’s doctor based on:
- Your child’s age, overall health and medical history
- Extent of the disease
- Your child’s tolerance for specific medications, procedures or therapies
- Expectations for the course of the disease
Early diagnosis and prevention of complications is critical in sickle cell disease treatment. Treatment options may include, but are not limited to:
- Pain medications
- Drinking plenty of water daily (eight to 10 glasses) or receiving fluid intravenously (to prevent and treat pain crises)
- Blood transfusions (for anemia, and to prevent stroke)
- Penicillin (to prevent infections)
- Hydroxyurea (a medication found to help reduce the frequency of pain crises and acute chest syndrome; it may also help decrease the need for frequent blood transfusions).
Bone marrow transplants for sickle cell disease
At Children’s National, we also have been able to cure sickle cell disease through bone marrow transplantation (BMT).
The first transplant for sickle cell disease happened at Children’s National in 1996 and our specialists have now done about 30 transplants. They started off helping the most severe patients, but now the push is to perform the transplant before the child has a stroke, which can happen in about 10 percent of sickle cell patients.
A child interested in BMT needs to be matched with the right donor within the family, usually a brother or sister, but only about 20-30 percent of patients find this right match. Before the BMT procedure, a child with sickle cell disease receives a high dose of chemotherapy to destroy their bone marrow to make room for new bone marrow to grow. Then, the patient receives an infusion of healthy bone marrow containing blood-forming stem cells. The new bone marrow produces healthy red blood cells and resolves the symptoms of sickle cell disease.
A multidisciplinary team of physicians, nurses, pharmacists, social workers, chaplains and physical therapists help guide families through the process of BMT. The entire BMT procedure requires hospitalization for about 5-6 weeks. Because the procedure is associated with very serious risks, parents can expect to answer a series of questions before enrolling their child to undergo BMT to cure him or her of sickle cell disease.
Parents with questions about sickle cell should ask their child’s pediatrician or check out Children’s National’s Sickle Cell Disease Program.
 https://riseandshine.childrensnational.org/wp-content/uploads/2020/02/Large-Group-of-People-Celebrating-feature.png
300
400
Rise and Shine
https://riseandshine.childrensnational.org/wp-content/uploads/2017/11/childrens_riseandshine_logo.jpg
Rise and Shine2024-02-27 07:00:312024-02-27 09:36:48Celebrate Rare Disease Day
https://riseandshine.childrensnational.org/wp-content/uploads/2020/02/Large-Group-of-People-Celebrating-feature.png
300
400
Rise and Shine
https://riseandshine.childrensnational.org/wp-content/uploads/2017/11/childrens_riseandshine_logo.jpg
Rise and Shine2024-02-27 07:00:312024-02-27 09:36:48Celebrate Rare Disease Day

 Allistair Abraham, MD, is a Blood and Marrow Transplantation Specialist at Children's National.
Allistair Abraham, MD, is a Blood and Marrow Transplantation Specialist at Children's National.


Leave a Comment
Want to join the discussion?Feel free to contribute!